Prior authorization transparency and reporting
Beginning in 2026, new federal rules require health plans to publicly share key information about their process and metrics for prior authorization (approval in advance for certain medical services). These changes are designed to give you clearer insight into how decisions
are made and how quickly requests are reviewed—so you can make more informed choices about your care.
Prior authorization metrics for medical items and services (excluding drugs) for 2025
The data in the reports below show which medical services require prior authorization; how many requests are approved or denied; and response and review times for standard and expedited requests.*
Standard (non-urgent) Prior Authorization Requests
|
|
How many times this happened
|
Out of total requests
|
Percentage
|
|
Total approved requests
|
14,127
|
15,445 |
91%
|
| Total denied requests |
1,318 |
15,445 |
9%
|
| Request approved within 14 days |
14,126 |
14,127 |
100%
|
| Request denied within 14 days |
1,307 |
1,318 |
99%
|
|
Approved after timeframe was extended (up to 14 days)
|
0 |
14,127 |
0% |
| Request denied after timeframe was extended (up to 14 days) |
0
|
1,318 |
0%
|
| Request approved after appeal |
120 |
178 |
67%
|
| Request denied after appeal |
59
|
179 |
33%
|
In 2025, Fallon Health received a total of 15,445 standard (non-urgent) prior authorization requests for our covered patients. 91% of those requests were approved.

The mean (average) time that it took to make standard prior authorization decisions was 3 days. The median (middle) time that it took to make standard prior authorization decisions was 0 day.
Expedited (urgent) Prior Authorization Requests (Response Due to Provider Within 72 Hours)
|
|
How many times this happened
|
Out of total requests
|
Percentage
|
| Total approved requests |
1,371
|
1,490 |
92%
|
| Total denied requests |
118
|
1,490 |
8%
|
| Request approved within 72 hours |
1,357
|
1,372 |
99% |
| Request denied within 72 hours |
103
|
118
|
87%
|
| Approved after timeframe was extended (up to 14 days) |
0
|
1,372
|
0%
|
| Request denied after timeframe was extended (up to 14 days) |
0
|
118
|
0%
|
| Request approved after appeal |
4
|
37
|
11%
|
| Request denied after appeal |
33
|
37
|
89%
|
In 2025, Fallon Health received a total of 1,490 expedited (urgent) prior authorization requests for our covered patients. 92% of those requests were approved.
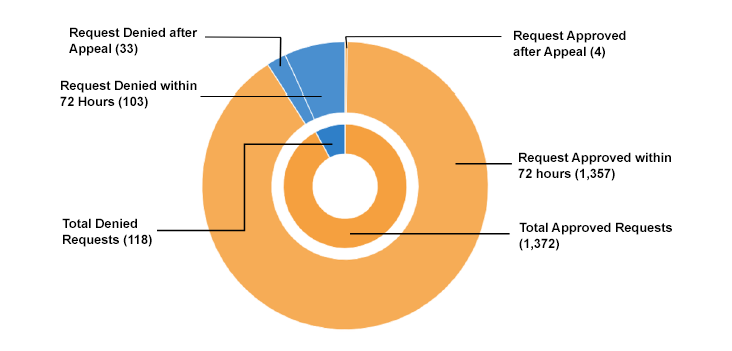
The mean (average) time that it took to make expedited prior authorization decisions was 17 hours. The median (middle) time that it took to make expedited prior authorization decisions was 3 hours.
Time Between Receiving a Prior Authorization Request and Sending a Decision
|
|
Mean (average) time
|
Median (middle) time
|
|
Standard (non-urgent) Prior Authorization
Requests (response due to provider within 14 calendar days)
|
3 days
|
0 day
|
|
Expedited (urgent) Prior Authorization Requests (response due to provider within 72 hours)
|
17 hours
|
3 hours
|
Health equity analysis
We want to make sure that everyone gets the same quality of health care, no matter who they are or where they come from. To help do this, the Centers for Medicare & Medicaid Services (CMS) is gathering data from health plans about how people are treated when they need prior authorization.
By studying this data, we can find out if some people are not getting the right care because of their social or health conditions and help make sure that everyone gets fair treatment.
You can view the report that Fallon Health provided to CMS below:
* Prior to January 1, 2026, prior authorization decisions were required to be made within 72 hours for expedited requests (urgent) and 14 calendar days for standard requests (non-urgent). Beginning January 1, 2026, prior authorization decisions are required to be made within 72 hours for expedited requests (urgent) and 7 calendar days for standard requests (non-urgent).
** This report represents the results of the CMS-required assessment of the impact of prior authorization on members who are defined as being potentially impacted by health equity inequalities versus those who are not defined as having health equity inequalities (as defined by CMS). The comparison shows no differential impact of prior authorization on members defined as being affected by health equity inequalities.
Call us toll-free at 1-888-340-5504 (TRS 711), 8 a.m.–8 p.m., Monday–Friday.
(7 days a week, Oct. 1–March 31)
H9001_260009_C_2026_B | The information on this page was last updated on 3/31/2025.